Android tablets
Stay up to date with the latest news, reviews, and buying guides for top Android tablets in a variety of sizes and specifications.
Reviews
Best products
Guides
Features
How-to's
All the latest
Android tablets news
I needed Samsung DeX to save me when my PC died, but it couldn't
Zac Kew-DennissMarch 9, 2025
0

The HONOR Pad V9 is a terrific tablet, but I don't know who will buy it
C. Scott BrownMarch 2, 2025
0

I turned my old Android tablet into a portable monitor, and you can too
Andy WalkerFebruary 27, 2025
0

The best Android tablets to spend your money on
Nick FernandezFebruary 17, 2025
0
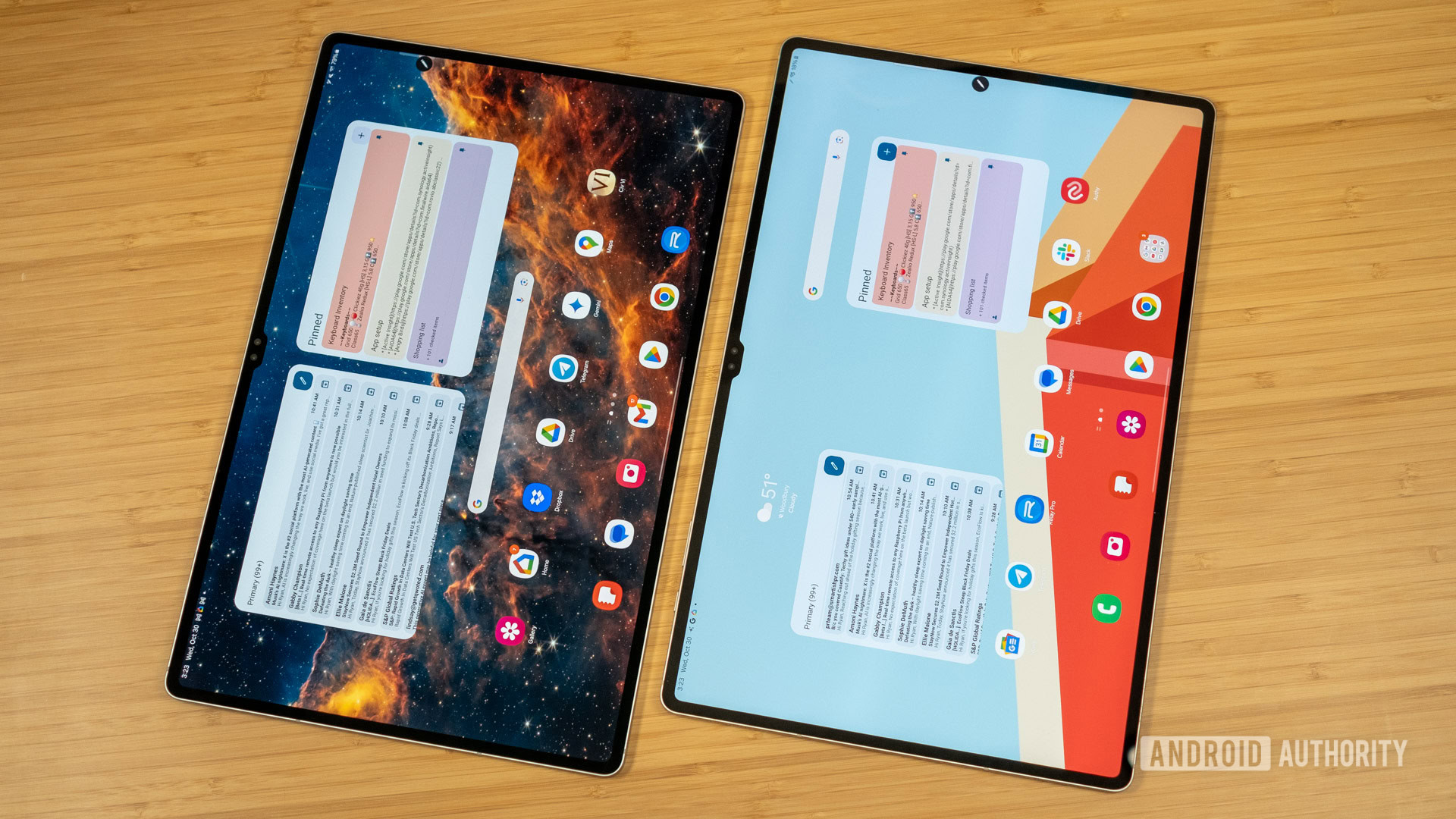
Samsung Galaxy Tab A9 Plus review: Should you buy it?
Ryan HainesFebruary 13, 2025
0


Download these cool wallpapers for your phone
Edgar CervantesFebruary 7, 2025
0

What's the best cheap Android tablet in 2025? Here are our top 8
Ryan HainesJanuary 27, 2025
0

The best E-Ink tablets: Do more than reading!
Edgar CervantesJanuary 27, 2025
0

Samsung Galaxy Tab S9 FE vs Galaxy Tab S9: Which Android tablet should you buy?
Andy WalkerJanuary 27, 2025
0

Samsung Galaxy Tab S9 FE problems and how to fix them
Ankit BanerjeeJanuary 23, 2025
0

We asked Google about the next Pixel Tablet at MWC 2025 and came away with this answer
Adamya SharmaMarch 4, 2025
0

Galaxy Tab S10 FE series leak sheds light on what hardware upgrades to expect
Ryan McNealMarch 3, 2025
0

TCL NXTPAPER 11 Plus tablet pricing looks as easy on your wallet as its screen is on your eyes
Stephen SchenckMarch 3, 2025
0

Renders for Samsung's upcoming Galaxy Tab S10 FE Plus leave nothing to the imagination
Pranob MehrotraMarch 2, 2025
0
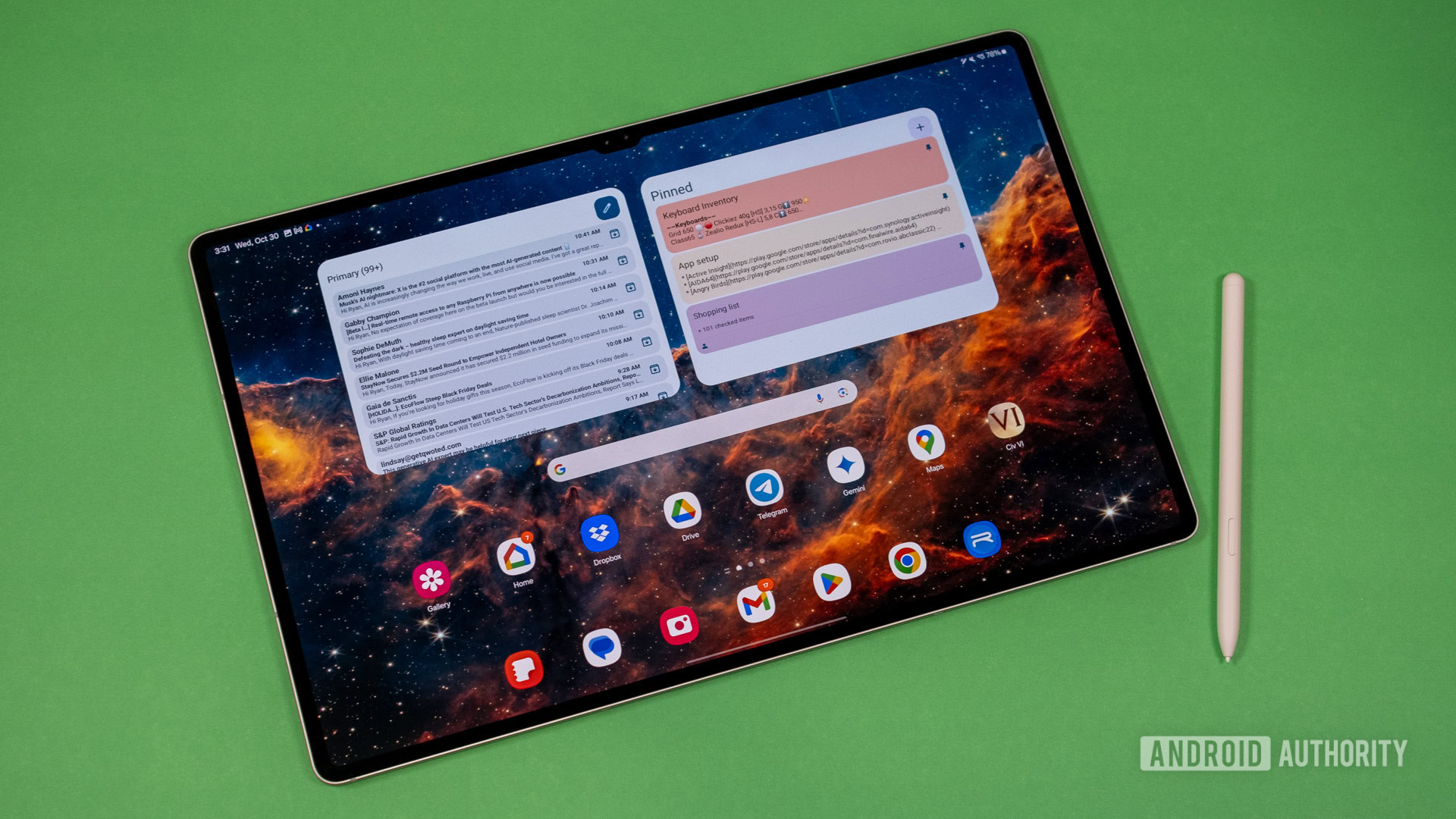
Galaxy Tab S10 FE Plus leak gives first look at Samsung's incoming tablet
Ryan McNealFebruary 28, 2025
0

Samsung could be rethinking its tablet sizes with the Galaxy Tab S10 FE series
Rushil AgrawalFebruary 26, 2025
0
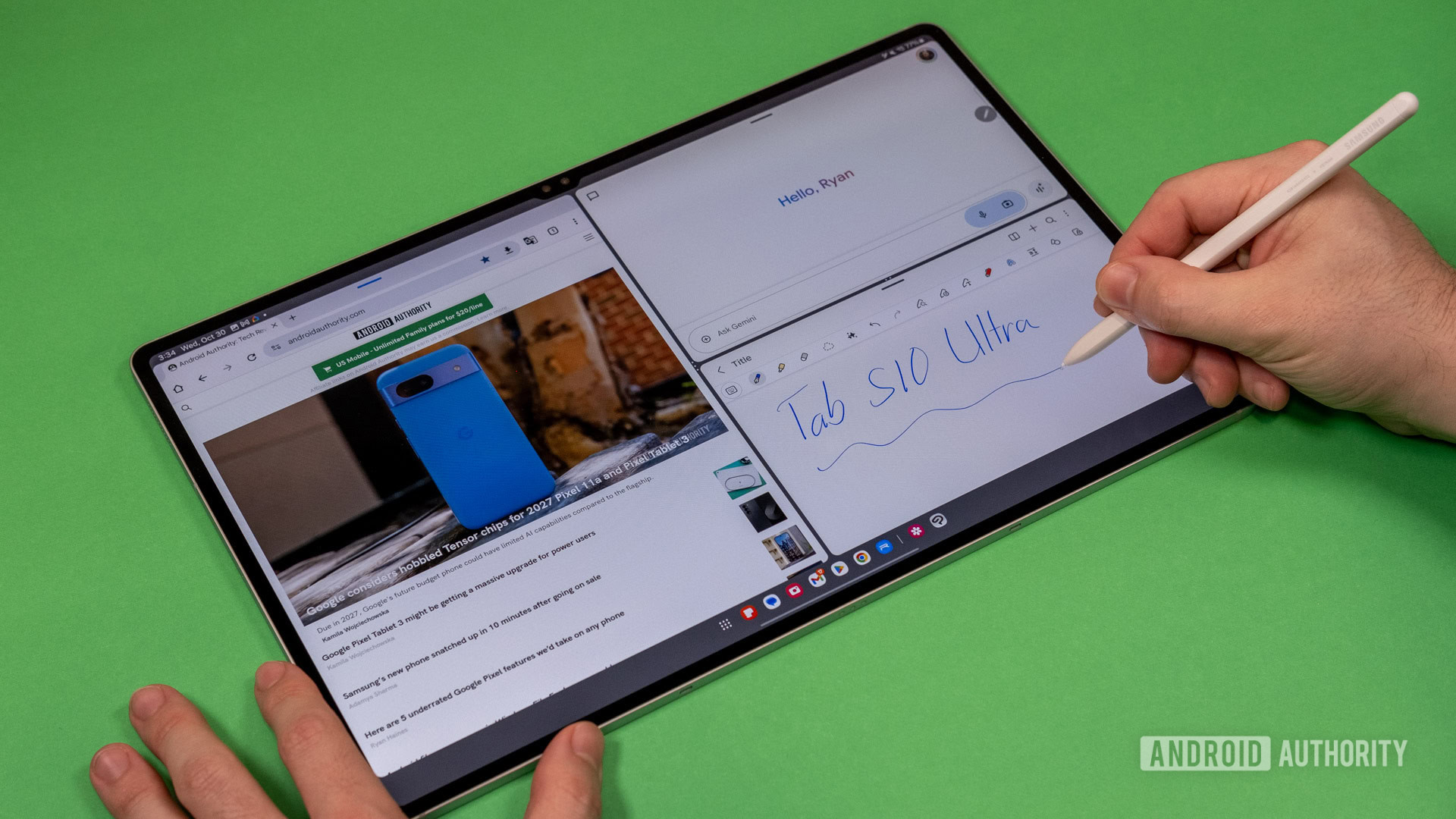
Qualcomm just got some real competition for this year's most affordable Android phones
Stephen SchenckFebruary 24, 2025
0

Google just gave Pixel owners a new choice when it comes to warranty plans
Ryan McNealFebruary 24, 2025
0

Love Android but hate Google? This Pixel Tablet is for you
Stephen SchenckFebruary 19, 2025
0

Apple iPad and iPad Mini go on sale; save up to $100
Edgar CervantesFebruary 10, 2025
0
